Inside The Manette Clinic’s Community-Rooted Direct Primary Care Model
In a healthcare system often defined by rushed appointments, fragmented care, and layers of insurance bureaucracy, The Manette Clinic in Bremerton operates on a different promise: give patients time, access, and a direct relationship with their provider. At its core, the clinic’s direct primary care model removes much of the traditional insurance structure in favor of something more personal, flexible, and transparent.
That shift changes everything about how care is delivered. Instead of billing codes and visit quotas, patients pay a membership fee that allows them to communicate directly with their provider, schedule longer appointments, and receive care without the constraints that often come with insurance-driven medicine. The result is a practice that prioritizes relationships over volume, prevention over quick fixes, and accessibility over complexity.
For founder Tanya Spoon, DNP, ARNP, FNP-BC, it’s not just a different way to run a clinic—it’s a different way to practice medicine.
“We’re not going to be millionaires,” Spoon said. “But I don’t hate my life. I love what I do, and I want to keep doing this as long as I can.”

From Burnout to a Different Model
Spoon’s path to The Manette Clinic grew out of her experience inside a traditional practice, where the pressure to see more patients in less time began to take a toll.
About 20 years ago, Spoon joined Dr. Minteer in Silverdale in what she calls “old-fashioned family practice.” “He was always on call. It was like old-fashioned family practice,” she said. “When I first started, I was seeing four or five patients a day and he was seeing 20. By the time we were done, I was seeing 25 and he was seeing six.”
“I was in it nine years with him and I felt tired,” she said. “I was 49 and I want to work until I’m 70. How am I going to sustain this? It was impossible—physically and emotionally.”
As hospital systems acquired small practices and reshaped local healthcare, Spoon saw a system moving further away from the kind of care she wanted to provide.
“I’ve lived here my whole life. Things were changing in my community,” she said. “There were lots of promises that they weren’t going to take over, but it ended up being kind of like a pirate ship coming in and taking over small practices. I didn’t want to be in that group.”
When an opportunity came to purchase the practice she worked in, she declined. Instead, she began searching for an alternative.
“There has got to be something different than this,” she said.
That search led her to direct primary care (DPC), a model that replaces traditional insurance billing with membership-based access.
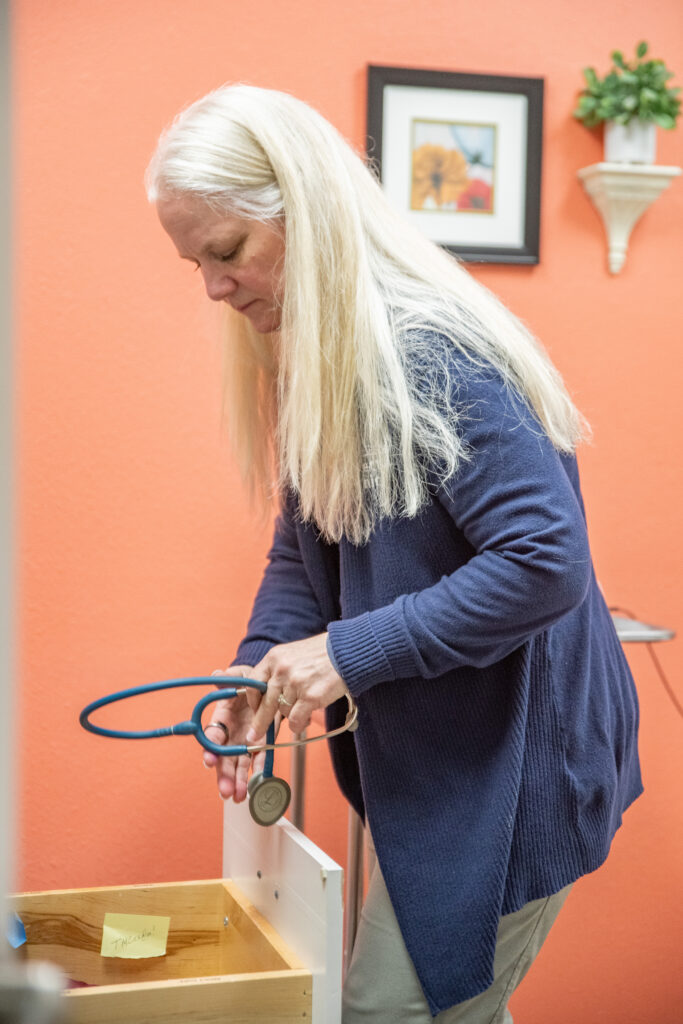
A Subscription Approach to Care
For Spoon, the distinction between direct primary care and concierge medicine is critical.
“The distinction between direct primary care and concierge is important,” she said. “Concierge practices are very expensive. It’s like your personal doctor who follows you to the hospital. Direct primary care is essentially membership-based medicine. Our patients can come see us whether they have insurance or not.”
The model is intentionally designed to serve a broad community—including people who might otherwise delay or forgo care.
“I’ve lived in Manette for 30 years,” Spoon said. “I asked myself, ‘What could the waitress at the Boat Shed afford? What could the person who runs the Manette afford?’ A lot of them don’t have insurance. When they get sick, they go to urgent care and spend $500. That’s not sustainable.”
To help understand and build the model, Spoon reached out to Dr. Garrison Bliss, a Seattle physician often credited as a pioneer of direct primary care.
“I started cold calling him,” she said. “They weren’t going to take my calls—silly little nurse practitioner wanting to start her own practice. Eventually, he took my call and carved out a couple of hours on a Saturday morning. I just asked him everything.”
His advice was simple and direct.
“He said, ‘You don’t have anything like this in your community.’ And I said, ‘I don’t.’ He told me, ‘Then you need to educate everybody.’”
Spoon took that advice to heart, speaking at Rotary clubs, community events, and health fairs to explain how the model worked and why it mattered.
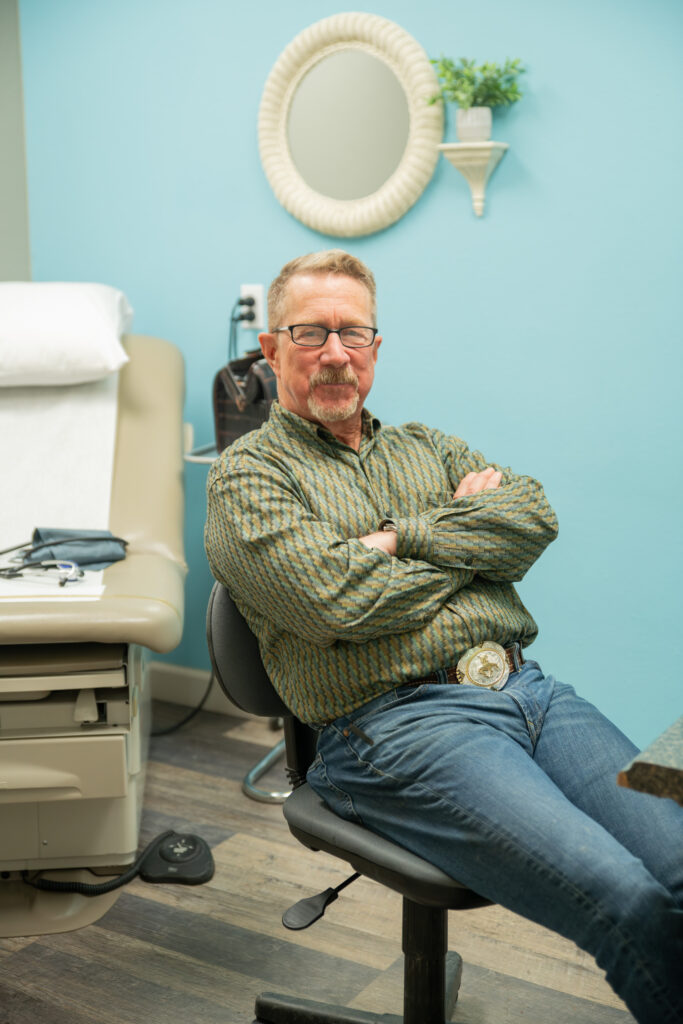
What Care Looks Like
For patients, The Manette Clinic still looks like a traditional doctor’s office—but the experience is different in key ways.
“It’s like joining a gym,” Spoon said. “You pay a membership fee to be able to come and see your provider. Everything’s up front and transparent. You know how much you’re going to pay every month, whether you use it or not—just like the gym.”
That monthly fee covers nearly everything done within the clinic, including check-ups, sick visits, and direct access to a provider, without billing insurance. Services sent out—such as lab work or biopsies—carry an additional cost, and patients benefit from discounted prescriptions, labs, and other services.
The structure allows the clinic to operate without the time pressures common in traditional practices.
“Because we’re a membership practice, our appointments are long,” Spoon said. “Our minimum appointment is 30 minutes. That changes the relationship. Our providers don’t have to run out the door in 12 minutes. We have the luxury of time.”
That time is foundational to how care is delivered.
“We get to know our patients,” she said. “I had a little girl in for an ear infection today and I asked, ‘How’s your mom? How’s her new job?’ I was actually her mom’s school nurse way back when.”
“Time builds relationship,” she added. “Because we have time, we can focus on prevention and overall wellness, not just treating illness.”
Access extends beyond the exam room. Patients can reach their provider through a dedicated text line monitored by the clinic, including weekends.
“Our patients have a line they can text us anytime,” Spoon said. “There’s always someone watching that, even on weekends.”
That accessibility allows providers to address concerns in real time, even when patients are away from home.
“We get things like, ‘My kid has this rash, what is this? We’re in Hawaii,’” she said. “Or, ‘I’m on a trip in Florida and I think I have a UTI.’ We can take care of those things. That’s a huge benefit for our patients.”

Balancing the Financial Equation
Spoon initially planned to operate a membership-only clinic without accepting Medicare, but patient feedback changed her approach.
“My patients were mad,” she said. “They said, ‘I’m on Medicare. What am I supposed to do?’”
Reluctantly, she added Medicare patients—and found it strengthened the model.
“Doing the combination of membership plus Medicare has been really beneficial,” Spoon said. “In that deductible season from January through March, when everything goes to Medicare’s deductible and we don’t make as much money, our membership holds us up. When membership is low, Medicare holds us up.”
Today, the clinic serves a wide range of patients, including those without insurance, those with high deductibles, Medicare recipients, and employees whose employers cover memberships instead of traditional health plans.
“Most people’s insurance has such a large deductible it’s almost like they’re not insured,” Spoon said. “Our fee is less than people’s deductibles.”

Growth Rooted in Community
When The Manette Clinic opened, Spoon wasn’t sure how many people would embrace the idea.
“I think I had like 30 people that came over, and I was nervous that more wouldn’t come,” she said.
But interest quickly grew.
“Pretty soon I had to start phoning friends to help me,” she said. “People were just coming out of the woodwork. Right now I have five providers.”
Even as the clinic has expanded, it has remained grounded in the community it serves.
“When the shipyard wasn’t getting paid, we held memberships,” Spoon said. “People could call us and say, ‘I’m having a hard time,’ and we’d say, ‘We’ll still see you.’”
That flexibility reflects the clinic’s commitment to accessibility—and its willingness to meet patients where they are.
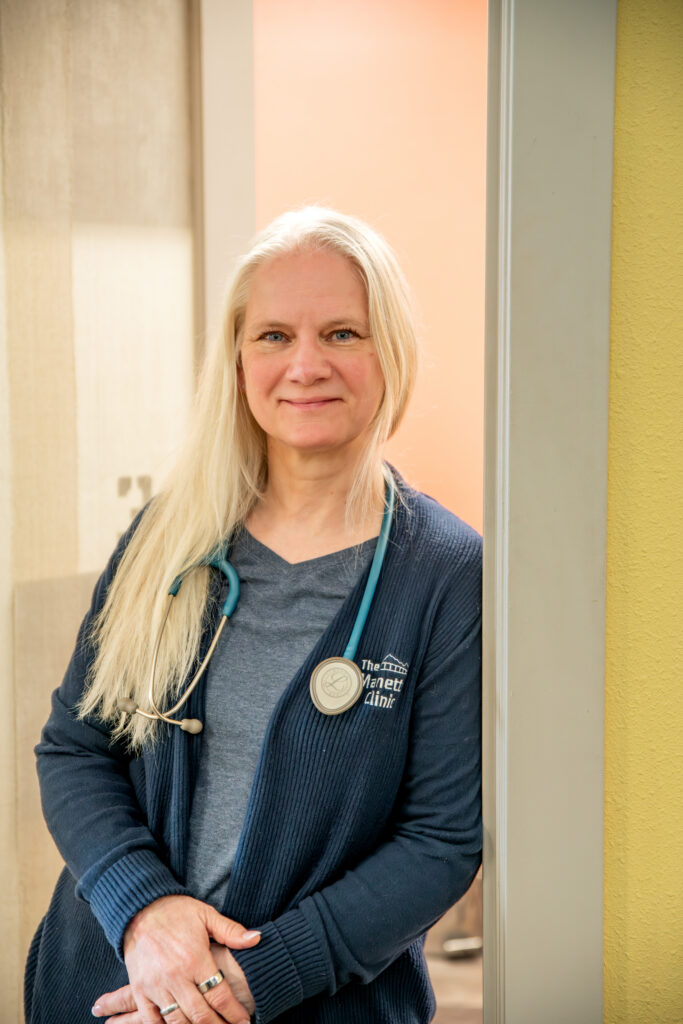
Time as the Core Value
At the center of The Manette Clinic’s model is time—both in and out of the exam room.
“Our Medicare wellness exams are 45 minutes to an hour,” Spoon said. “We ask, ‘Do you have a living will? Do you have a durable power of attorney?’ We want people to be well cared for all the way to the end of life.”
That level of attention would be difficult to sustain in a high-volume, insurance-driven practice, she said.
In contrast, The Manette Clinic avoids quotas tied to patient volume.
“The quota at one large system’s specialty clinics right now is 100 people a week,” Spoon said. “That’s not sustainable.”
Instead, providers at The Manette Clinic work full time at around 30 hours a week, with flexibility built into the schedule.
“There’s nothing strict about this format,” she said.
The clinic also incorporates complementary approaches alongside traditional medicine.
Spoon is certified in acupuncture, and the team offers functional and hormonal medicine services as part of their care.
“I felt like, What else can I give my patients without writing them another prescription?” she said.

A Practice Built on Relationships
For Spoon, the most meaningful measure of success isn’t growth or revenue—it’s connection.
“I see five generations of families,” she said. “I’ve seen them for 20 years.”
That continuity allows her to care for patients across their lives—from childhood to aging.
“It’s pretty cool,” she said.
As healthcare continues to consolidate, Spoon knows practices like hers are becoming less common.
“We’re losing something if we lose our local primary care offices,” she said.
Still, she believes the model has a future—especially in communities like Kitsap County.
“In a community like ours, something like this is very appreciated,” she said. “It’s not easy—but it’s worth it.”
Keep in touch with our news & offers
Subscribe to Our Newsletter
Thank you for subscribing to the newsletter.
Oops. Something went wrong. Please try again later.









